
Making Gravity Work For You
September 28, 2011
By Dr. Ryan Nomura


Dr. Ryan Nomura
Physiatrist at Rehabilitation Hospital of the Pacific
Where did you receive your schooling and training?
For college I went to Northwestern University in Evanston, Ill., and then I went to the Northwestern University Medical School in Chicago. I did my medical internship at Saint Louis University and my residency in physical medicine and rehabilitation at UC-Irvine in Orange, Calif. I started working here at REHAB Hospital straight out of residency in 2008.
What are your responsibilities as medical director of the orthopedic program?
At REHAB we treat a wide range of patients which include strokes, brain injuries or other traumatic injuries, and have traditionally treated a large number of patients with orthopedic conditions, such as post-operative knee or hip replacements. But lately because of the changes in insurance coverage we are seeing an increase in more complex patients with fractures and other traumatic and neurologic injuries. Nowadays, a patient has to have a certain level of medical necessity to warrant a hospital stay at an acute rehab facility for post-operative care. A part of my job is to determine the level of care needed for patients who are referred to us for example, whether or not they will require an inpatient admission versus going to an outpatient clinic. I also work with our team of rehab nurses, therapists and case managers to oversee the rehab and medical treatment of those patients admitted to the REHAB Hospital under my care.
{embed=“elements/box_ad”}
Can you talk about the range of treatment you offer?
At REHAB we have an inpatient hospital facility where we provide medical care and a minimum of three hours of daily physical therapy, occupational therapy or speech therapy. This is where we treat our more acutely ill or post-operative patients. We also have outpatient therapy clinics for those who have “graduated” from our inpatient program, or for community referrals for musculoskeletal injuries. Our clinics also offer aquatic pool therapy and Pilates, as well as some of the latest technology in rehab care like the AlterG and the Tibion Bionic Leg.
|
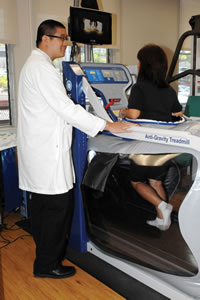
What is the AlterG and the Bionic Leg?
The AlterG is an antigravity treadmill. We have the patient put on neoprene shorts, kind of like biker shorts, and we zipper them into a contraption that is like an inflatable balloon that unweights the patient. It can eliminate up to 80 percent of the patient’s body weight and can increase the load by 1 percent increments, so there’s a very high level of control in terms of what weight you want the patient to bear. The benefit of this is you can have people doing a more physiologic type of exercise sooner after surgery than you would in most cases. It improves circulation and allows for earlier active range of motion exercises, which is for good neuromuscular reeducation, and minimizes joint stiffness.
What conditions does the AlterG help with?
A lot of times after a hip fracture or hip or knee replacement surgery, you have lots of inflammation. Inflammation is the body’s natural physiologic response to trauma. It causes an increase in circulation, assists in tissue repair and combats infection. The problem is there’s some deleterious effects of inflammation over the long term. It causes pain. It causes the patient to guard or protect the affected limb and not use or walk on it. When people don’t use the muscle or don’t walk and don’t mobilize the joint, they can develop scarring, stiffness and muscle weakness. Over the long term, this can negatively impact their walking pattern, their body mechanics. It’s going to cause more problems and more wear and tear on your other joints trying to make up for the deficit that you have on the affected leg. The benefit of having people use the AlterG earlier in their recovery period is it allows for early joint mobilization, neuromuscular re-education, muscle strengthening and normalization of gait mechanics to reduce the need for assistive devices. There’s a camera that takes a video of the patient’s legs and their feet when they’re walking so they can get visual feedback in terms of what they’re doing wrong. They find that very helpful.
The Lakers, AC Milan, Manchester United they all have an AlterG as part of their rehab programs for their athletes.
{embed=“elements/google_ad336x280”}
How does the Bionic Leg work?
It was designed for use in post-stroke patients, but we’ve found that it also works really well with orthopedic patients, like those who have had kneereplacement surgery. It augments knee extension and helps with the walking pattern. There are some sensors in the footplate and it detects pressure when you put weight on the leg. When you put pressure on the front part of your foot and the device detects the knee straightening, the motor kicks in and it helps you with knee extension to strengthen and stabilize the leg. When you start bending the leg, it senses that the knee is bending and it provides a braking force to control you in your descent. So it gives patients a lot of confidence when they’re walking. It helps when they’re going up and down stairs. This really augments their leg strength when they’re doing therapy or their exercises. When they come here to use the Tibion and the AlterG, they come for maybe an hour or two, two or three times a week. We also provide them with a home exercise program to help maximize their benefit from formal therapy.
Any other latest advancements?
Right now we are awaiting our eLEGS exoskeleton walking frame that will allow paraplegics to walk. We are one of very few facilities in the nation to have this technology. It’s a very exciting time it’s like the technological revolution. Sci-fi things from when we were growing up like bionic legs and cyborgs - you can kind of see that come to reality nowadays.