Coming Back From A Stroke

Interviewed by Lisa Asato
Wednesday - August 08, 2007
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share
First of all, what’s the goal of stroke rehabilitation?
Particularly after a stroke, there can be deficits in a person’s ability to walk, in their mobility ... They may have difficulties with speech, memory, problem solving, ability to dress themselves. ... So we’re involved in the rehabilitation process to look at all of those areas to either compensate or to help regain function to allow them to be as independent as possible.
So the degrees of help needed could really differ?
Usually it depends how big the stroke was and where in the brain it was located. ... Sometimes it can be very minor - they may have just some slurred speech. It can range to complete hemiplegia (paralysis on the right or left side of the body) or if the stroke is on both sides of the brain you can have it affect all of your limbs. It can affect your cognition, your swallowing. You can end up basically being bedridden so there’s a very large range. Some people, after a small-enough stroke, can go directly home and just get therapy as an outpatient.
|
How prevalent is stroke in Hawaii?
Stroke is the third-leading cause of death in the U.S. and in Hawaii. ... The mortality rate for Hawaii is 53 per 100,000.
Is there a certain age group this is more common to?
Age in and of itself is a risk factor for stroke, so after the age of 55 for every decade your risk of stroke about doubles for every decade you go past 55. So as you get older your risk of stroke increases.
How many of Hawaii or Oahu stroke patients come here for rehabilitation?
It’s tough for us to say, (but) I can tell you that last year we saw over 300 stroke cases here and about one out of every five admissions here is a stroke admission. ... so it’s a very common diagnosis for us.
What’s unique about stroke rehabilitation at your hospital?
The Rehab Hospital of the Pacific is the only acute in-patient rehabilitation facility in the state. In order to qualify to come here you need to have a multidisciplinary need - that means you need rehab in more than one area so you can’t just need physical therapy. You need to have physical therapy and occupational therapy or physical therapy and speech therapy.
Are there other requirements?
You need to be able to tolerate three hours of therapy a day. So sometimes people are either too good or too sick to come here.
What other specialties do you offer besides physical, occupational and speech therapy?
We also have neuropsychologists here as well who deal not only with cognition but will help people to cope with emotional aspects after the stroke. We also have recreational therapy, which has pet therapy and social activities for patients. We also have a stroke club that people can go to as an outpatient (call Kate Church at 566-3791), and we have case managers that help people arrange for aftercare to help deal with insurance issues.
Did you say pet therapy?
As part of our recreational therapy we have Simba, a golden retriever, who is our resident pet therapist. He is actually taken care of by two of our therapists here, Mike Ebesu and Dawn, his wife. Simba comes to work five days out of the week and he works two hours a day. But he basically will go around, just say
‘Hi’ to patients and let them pet him and see him. It really is an emotional boost for a lot of people, especially people who miss their pets, and it’s something that they can pet and hug and feel OK about to get some kind of support.
Can you describe a common disability caused by stroke?
Spasticity is an increased stiffness in the arm or leg where people will have a hard time moving their joints and will often tend to stay in a certain position. ...
If you’re constantly in one position all the time your joints can get stuck that way (contracture) so it’s very important for people to do exercises where they try and get a full range of motion in all their joints.
Being stuck in a certain position all the time can also cause pain, and if, for instance, your hand is stuck in this position (fist) you can’t clean it very well so it becomes a hygiene issue. Your fingers can get so tight to the point where your fingernails will dig into your palm. It’ll cause injury and actual skin breakdown.
If it’s in your legs and your legs tend to cross over they’re so tight it can be hard to urinate or to clean yourself. There’s medication for that, but there’s also Botox, you know Botox that people will use for wrinkles in their face? Botox can also be used for spasticity.
What it does is it affects the muscle so that they can’t contract as tightly and so it helps to loosen that. If it’s a specific area that’s causing trouble. Botox is a good thing because it’s localized to that area. You do have to repeat the treatments about every three months or so.
What are some new techniques in stroke rehabilitation?
Traditionally what we would do is what we call mat exercises - we try and work on strengthening and range of motion before we would attempt the standing and walking. Now we’re pushing to start that standing and walking as early as possible.
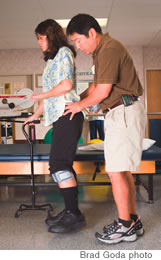
What is Bioness (shown in photo)?
Bioness is a functional electric stimulation (FES) that looks like a brace on either the arm or the leg, and it applies an electrical impulse or stimulation to the muscles and nerves in the arm or leg. ... It helps to strengthen those muscles, encourage those muscles to regain their function so that, hopefully, patients won’t need as much bracing or won’t need bracing at all eventually. ... We are the only ones in the state right now that have this system.
There’s also - its not a Bioness system - but its also electric stimulation, called VitalStim that helps for swallowing, its to help strengthen the muscles for swallowing.
You’re a physiatrist. Can you describe the field?
We’re not a commonly known field, but basically we are physicians that specialize in the field of physical medicine and rehabilitation. That’s what we’re also known as: PMNR.
How long have you been doing this kind of work?
I’ve only been working here since January. I just finished my residency last July at Mount Sinai Medical Center in New York City, so I was there for four years. I am a graduate of the John A. Burns School of Medicine.
This information is provided as educational and is not intended as a substitute for consultation with a physician. For questions, consult your physician.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):