Diagnosing Sleep Disorders
Interviewed by Guest Writer
Wednesday - May 20, 2009
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

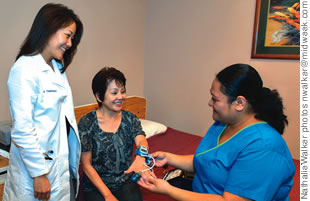
Dr. Shanon Takaoka
Medical director of Kaiser Moanalua Sleep Laboratory
Interviewed By Melissa Moniz
Where did you receive your schooling and training?
I graduated from Baldwin High School on Maui and did my undergraduate degree in human biology at Stanford University. I came back to Hawaii and attended the UH John A. Burns School of Medicine. I did my internship and residency in internal medicine at Cedars-Sinai Medical Center in Los Angeles, followed by fellowships in pulmonary, critical care and sleep medicine back at Stanford.
Can you talk about the sleep lab and the services that it offers patients?
The primary role of the sleep lab is to diagnose sleep disorders - mainly sleep apnea, but we also can detect a variety of other disorders like restless legs syndrome, periodic limb movement disorder, sleep walking, sleep talking, teeth grinding and, to some degree, insomnia. Our primary goal is to identify, evaluate and treat anyone who is experiencing disrupted, poor-quality sleep.
An important service offered only at the Kaiser Permanente Sleep Lab is sleep education. Prior to any sleep study, patients attend an educational session at Kaiser Moanalua. This seminar is led by the medical director of the sleep lab and combines clinical assessment, limited airway evaluation and a 30- to 40-minute discussion that covers basic sleep facts and myths, reviews sleep studies and what to expect, provides an in-depth overview of sleep apnea, and provides a question-answer opportunity to patients.
Can you explain what the Watch-PAT is and how it has helped in diagnosing sleep disorders?
The Watch-PAT is a very simple, accurate and compact way of diagnosing sleep apnea, specifically. The device looks like a simple wristwatch that the patient takes home and puts on at bedtime. The Watch-PAT takes data from a patient’s blood pressure changes, heart rate and breathing during sleep in order to detect sleep apnea. This new technology has been available for less than two years and was only recently approved by Medicare. Kaiser Permanente’s Moanalua Medical Center is the only sleep lab in Hawaii that is using this device.
The benefit of the Watch-PAT is that it provides patients who may have difficulty falling asleep in the sleep lab the means to have a sleep test done in the comfort of their own homes. It’s so small and easy to use that it is much less intrusive than typical sleep testing and doesn’t interfere as much with a patient’s normal sleep patterns. It is also helpful in people who are shift-workers or have unusual sleep schedules, as well as those on the Neighbor Islands who may have less access to in-lab sleep testing. By using the Watch-PAT in selected patients under these circumstances, we are able to mimic their normal sleep environment to the best of our ability, which makes the test that much more accurate.
|
Is there anything that you can do in the sleep lab that the Watch-PAT can’t do?
While the Watch-PAT is great and affords some advantages in select patients, the information we obtain is more limited compared to traditional sleep testing and is specific to the diagnosis of sleep apnea. When people come into the sleep lab, we monitor many more body functions during sleep, including brain activity, heart rhythms, breathing, eye and leg movements, and even video. We are able to integrate all of this information in order to diagnose more-complex sleep disorders that Watch-PAT will miss. The sleep lab also is the most-accurate and safe way to evaluate patients with more-complicated medical conditions such as heart or lung diseases, or those taking many different types of medications.
Is it true that many people suffer from sleep disorders but aren’t aware of it?
Yes, sleep disorders affect an estimated 70 million people across the U.S. Unfortunately, both patients and physicians often fail to recognize or even talk about the symptoms. People often blame their disrupted, poor-quality sleep on busy work schedules, family responsibilities and demanding lifestyles. Many of us take sleep for granted and don’t recognize how important good-quality sleep is until it’s gone. And good-quality sleep is sleep that is restful and uninterrupted. With awareness and education, doctors and patients are getting better at identifying and discussing symptoms of sleep disorders, and our tools to detect them such as the Watch-PAT are improving our ability to make these diagnoses.
Is there a direct correlation between sleep apnea and obesity?
Absolutely. Although you don’t have to be obese to have sleep apnea, obesity is one of the biggest risk factors for developing sleep apnea. As our population becomes more obese, the rate of sleep apnea will continue to rise. So weight loss becomes a key element in the treatment of this problem.
Aside from obesity, what are other risk factors for sleep apnea?
Sleep apnea is actually a problem of the internal airway that we breathe through. That airway is really just one long tube made primarily of muscles that run from the nose, down the back of the throat and into the lung. People with sleep apnea tend to have smaller, more collapsible airways that they inherit from their parents and pass on to their children, just like features like height or eye color. As a result, sleep apnea is a problem that tends to run in families and in certain ethnic groups such as Asians and Pacific Islanders. Older age, male gender and a large neck size also are well-recognized risk factors for sleep apnea.
Around what age does sleep apnea usually present itself?
Because sleep apnea is a disorder related to the airway, it can actually be present from early childhood. However, it is more common for this disorder to be noticed later in life. In men, it tends to become apparent right around the time of puberty, mainly because testosterone increases during this time, which leads to increased muscle mass and weight gain. Those two things contribute toward sleep apnea by increasing airway crowding. That’s usually when you start to hear snoring in men. Women actually have a much more delayed presentation of sleep apnea - it tends to happen right around the age of menopause. Hormone levels start to drop, which leads to loss of airway muscle tone and increased airway collapsibility during sleep. Menopause also is a time when metabolism decreases and women tend to gain weight, which is an added risk factor for sleep apnea.
What are some simple lifestyle changes that people can do to get a better night’s sleep?
Getting refreshing sleep depends on two simple but important factors. The first is quantity, or how much sleep you get each night. The second is quality, or how good that sleep actually is. First and foremost, it’s always important to get enough sleep. Although the amount varies from person to person, an average of seven to nine hours per night is recommended.
On the quality side, it’s important to create an environment that is conducive to sleep - the bedroom should be kept dark, quiet, at a comfortable temperature, and should be reserved for sleep and sleep-related activities. Things like TV-watching and reading should be done in another room prior to bedtime.
It’s also helpful to realize that large meals, caffeine, nicotine, alcohol and sedatives (such as pain medications or sleeping pills) can interfere with the quality of sleep and should be avoided prior to bedtime if possible. Regular exercise and avoiding naps also improve nighttime sleep quality.
What other treatment options are available?
The primary treatment for sleep apnea is CPAP (Continuous Positive Airway Pressure). This is a device that delivers pressurized air to the upper airway to keep it from collapsing during sleep. By keeping the airway open, CPAP allows the patient to breathe normally and maintain normal sleep patterns throughout the night. It is safe, painless and relatively non-invasive. CPAP has very few side effects, but is a process that takes getting used to. When it is being used regularly and working well, CPAP is the most effective treatment available for sleep apnea.
Is the CPAP a temporary fix to the problem?
Yes, anytime CPAP is not used sleep apnea comes right back. It isn’t a definitive, long-term treatment and must be used every night for the whole night of sleep for it to work. Throat surgery is a second-line option for selected patients. Unfortunately, it only effectively treats sleep apnea about half the time. In those 50 percent of patients who do benefit, surgery can be a definitive cure.
Are there any new breakthroughs on the horizon that will help in better treating sleep disorders?
I think there are a lot of people trying to look for alternatives to the existing sleep apnea treatments because the options we have, namely CPAP, are effective but are inconvenient, bulky and not definitive. It is clear that we need treatments for sleep apnea that are easier to use, just as effective and better at treating this disorder in the long term. Although there are no clear solutions currently, this is a major area of active research in sleep medicine with the promise of treatment alternatives on the horizon.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):