High-tech Prostate Treatment
Interviewed by Rasa Fournier
Wednesday - December 29, 2010
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

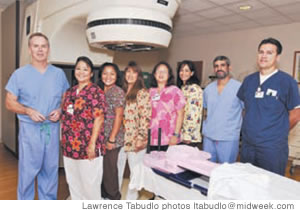
Dr. John Lederer
Radiation oncologist and medical director at The Cancer Center of Hawaii
Where did you receive your schooling/training?
I’m from Texas and went to medical school at Baylor College of Medicine in Houston, at the Texas Medical Center. I’m also board certified in internal medicine and I taught a bit of internal medicine before I went into radiation oncology. I did my radiation oncology at the University of Utah in Salt Lake City, then I moved to Hawaii in 1989.
How long have you been practicing?
Since training, it would be 21 years.
How does your new machine for treating prostate cancer work?
This Calypso device has a unit that transmits and receives discrete frequencies to and from Beacons that I place into the prostate. The Beacons allow us to do two things that are much more difficult to do in their absence. No. 1, every day when we initially line up the treatment beam, we know exactly where the target is, because 10 times a second these Calypso Beacons are sending out a frequency. It’s not just based on where the target was the day you did your three-dimensional planning which, in fact, could even be 2 or 3 centimeters off. So, we can localize it at the beginning of each treatment. Secondly, we can set parameters, and if the prostate moves during the treatment, which it does quite often and it exceeds those parameters, the machine alarms and we can recenter the treatment to account for the movement.
How do you implant the Beacons?
If a patient has prostate cancer, the vast majority have had a prostate biopsy, which is usually an outpatient procedure in which an ultrasound is placed into the rectum to visualize the prostate, and the biopsy is performed through the rectal wall. I’ve personally had a biopsy, so I can relate. Implanting the Beacons is very similar. Instead of removing tissue, as in the biopsy, three rice grain-size Beacons are placed into the prostate.
How do the Beacons identify the cancerous area?
They identify the prostate. Two-thirds of the time, if you remove the prostate after the biopsy was performed, one would find there’s cancer in more areas than you knew about, so we treat the whole prostate. With treatment such as seed implants, there is a little higher dose delivered to the cancerous area identified on the biopsy.
With traditional prostate cancer treatments, we remove the whole prostate or we radiate the entire prostate. By putting these Beacons in the prostate and then computer planning around that, we know where the prostate is. We also know where the rectum and the bladder are, so we can protect them better while at the same time making sure that the beams are actually hitting the prostate.
Unlike the computer plans without the Beacons, where we just have to assume every day that the patient’s prostate is in more or less the same spot, and also assume that it’s not moving during the treatment, with the Calypso we can, within .2 millimeters, be exactly on target. And if it moves outside of your parameter more than 3 millimeters, we recenter the beam. The Calypso offers a much more precise treatment, and studies have shown that even with giving a higher dose, the patients have fewer side effects.
|
How long have you been using the Calypso?
We put in our first Beacons in March. We wait a couple of weeks for the prostate swelling to go down after implanting the Beacons, and then perform computer planning. I think the first patients started in April, and we’ve implanted about five sets of the Calypso each month.
For a fairly small place like Honolulu, five a month indicates good patient acceptance of this technology. And it’s picking up because more and more patients hear about it and they understand the logic of it. Occasionally people say, “Well, Doc, I just don’t want to do that,” and that’s OK.
Using the Calypso has its advantages, but if we didn’t have it here, should a patient go to Los Angeles to get this done? I’d say no. It’s probably not that big of an advantage that patients would like to relocate to the Mainland for two months. However, if this is available in town, it makes perfect sense to utilize the increased accuracy made possible by Calypso. The Cancer Center of Hawaii is the only Hawaii facility offering Calypso.
Does the machine only treat prostate cancer?
We have a machine called a linear accelerator that is utilized to treat cancer in any part of the body.
The FDA has approved the implantation of Calypso markers into the prostate, including for patients who have had prostate surgery, but still need radiation after the surgery.
Calypso is theoretically the ideal thing for lung cancer because as a person breathes, the lung cancers move up to several inches. The pancreas is another organ in which Calypso may be utilized in the future. If we can make the radiation more accurate, it becomes more effective and safer, and that’s always our goal.
I treat a lot of prostate cancer - that’s why I wanted the Calypso, and I have friends on the Mainland who treat a lot of prostate cancer. I contacted them, and asked, ‘Hey, does it really work the way it’s supposed to, and it’s not just some sort of hype that doesn’t really do anything?‘and they’d say, ‘Oh, yeah, we’re really pleased with it.’ These are guys who specialize in prostate cancer, it’s not like they just dabble in it. If they’re pretty happy with it, you can be pretty certain that it works. So that’s when we made the leap. It’s always a challenge to get a new technology up and running.
Our goal is to be able to deliver the best care we can so our patients don’t have to go off to the Mainland. I think, for prostate cancer, it’s hard to beat this for any kind of external radiation.
There are other kinds of radiation where you put radiation directly into the prostate, and those have their advantages and disadvantages too, but if you need to, or if the patient chooses to take external radiation, this is clearly a new level above in improving accuracy.
Can the patient continue normal activities after the procedure?
Yes. People getting these kinds of daily radiation treatments can go back to work, can drive a car, take their regular medicines. If they’re a golfer, they still go golfing.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):