Joint Pain And Inflammation
Interviewed by Rasa Fournier
Wednesday - January 26, 2011
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

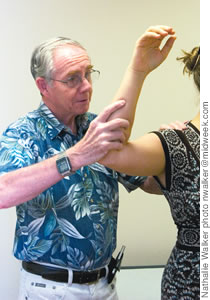
Dr. Dennis Crowley
Physiatrist at The Queen’s Medical Center
Where did you receive your schooling and training?
At Creighton University in Omaha, Neb.
How long have you been practicing?
I graduated from medical school in 1968 and I have been practicing in Hawaii since 1976.
What does a physiatrist do?
Physical medicine. Many of our pain conditions are caused by repetitive stress and force. Repetitive stress often-times results in repetitive friction, and friction, if it happens a lot, results in inflammation. If it happens on the skin, we see it as a blister. If there is friction in a joint, it swells and gets red hot and sore and painful. And that’s what a lot of people encounter in the course of their life - inflammation and pain in the area of the back and joints. Repetitive friction where bones meet results in joint inflammation, which results in arthritis. Arthritis is basically a joint blister. To reduce pain, we try to reduce the amount of inflammation.
What do you do to treat inflammation?
The most important way is learning to avoid creating friction. There are a lot of arthritic drugs. Many patients don’t want to take man-made chemicals, but anything that goes into our mouth ends up a chemical once it hits our stomach. So often people say they’ll only take medicine once it’s really bad, at which point the medicine won’t be able to help them much, because the pain is already bad. What they ought to take for osteoarthritis is arthritis medicines like Motrin and Naproxen. They are anti-blister, anti-inflammation medicines. They try to calm down the pain and inflammation. They are not addicting. They are generally safe. There are some side effects to watch for, but every medicine has side effects. They are not opioids/narcotics - those have limited effects.
|
Opioids do not do anything to treat the inflammation. They may blunt the feeling of pain. They often help only a little bit and they have a number of side effects. The biggest one is that one can easily become dependent upon it. The contradiction there is that, if someone’s on opioids for a long period of time, their body re-adjusts and they become actually more sensitive to painful stimuli than if they were off of it completely. We’re having more suicides due to opiate overdoses. It’s been a steady trend over the last 10-15 years. I think people need to be very cautious with those medications. They fall short of helping. They also numb the brain a bit, and numb brains don’t deal with life’s stresses very well. It gets in the way of good problem-solving.
How has physical medicine, or physiatry, changed since you’ve been in the field?
The biggest change was in the ‘80s. Specialists in physiatry started doing interventional treatments. With the guidance of Xray, they would place medicine right at the site of the pain generators, generally in the low back and sometimes in the neck. That’s not something I do.
What conditions do you treat besides arthritis?
Conditions resulting in pain in the neck, shoulders, hips and knees. Another group of patients come because of impairments due to stroke, spinal cord injury, amputation or recovery after bad fractures. They benefit from physical therapy to help them move along. To maximize their community involvement, they may need assisted devices such as power chairs, artificial limbs and braces.
Polio patients can be commended for their resolve to be as active as they can be, and part of that is to try to fit in, to look normal. In their childhood, they become very good strugglers and very persevering, and they achieve a lot both physically and in the world of work. But aging catches up with them, so what was working - what may be a very abnormal gait, but they were still walking - they reach a wall where they just can’t do it anymore. It’s a very hard adjustment for them to think about having to rely on a wheelchair for their mobility.
They can fight it, but life is a marathon of repetitive stress, and the logical way is to say I’ll use a wheelchair some of the time to get more mileage out of my bad knee or my bad hip, but only one out of 10 such patients goes ahead and does that. Others just keep plugging away and grinding in their shoulder joints or grinding their hip and knee joints. We work with them and talk to them about adjustments, and because they are in charge of their health, they’re going to do what they want to do.
Can you talk about some of the latest advancements in the field?
Electrodiagnostic studies, which operate on the principle that the body generates its own current. That’s what makes a muscle contract, that’s how you end up seeing the EKG (elcotrocardiogram). That’s simply reflecting the flow of current across the muscles of the heart. So we’re able to connect the machine to the body. And then we start seeing the flow of current in the reactivity of muscle.
The biggest advancement is in the area of imaging with the MRI and other types of imaging like nuclear scan imaging. It helps us identify where the basis of the pain is. There are always going to be some signs of degeneration, some collapsing or bulging of the disc. What’s critical is, does it bulge into a nerve and put pressure on a nerve? Or is it mostly all an arthritic reaction in the spine, without nerve damage, in which case surgery is not helpful? If there’s definite damage to the nerve, then surgery may well be the treatment of choice.
Nerve conduction studies help us document the function of the nerve. You can take an MRI of an arm in a person who’s not alive and you’ll still get a picture, but what you really want to know is, not just the anatomy, but whether the nerve is functioning. Nerve conduction studies show whether the nerve is working or damaged, and is it damaged a little bit or a lot. We do that with nerve flow studies and by searching in the muscle for signs of injury, or studying the muscle reactivity to see if the activation is normal, or is the wave form abnormal. We can tell if someone has a muscle disease versus nerve damage as a basis for weakness.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):