Meth Causing ‘Young Strokes’
Interviewed by Rasa Fournier
Wednesday - February 16, 2011
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

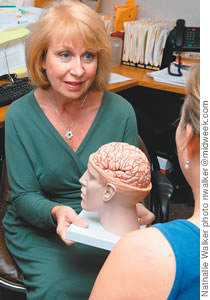
Dr. Nancy Lamport-Hughes
Clinical rehabilitation psychologist at Rehab Hospital of the Pacific
Where did you receive your schooling and training?
My undergraduate work was at the University of Minnesota and my graduate work was at Saybrook Graduate School and Research Institute in San Francisco. I came to the Rehabilitation Hospital of the Pacific in 1991.
How long have you been practicing?
More than 25 years.
Can you talk about your young stroke patients?
The primary responsibility of the Rehab Hospital of the Pacific is to provide rehabilitation services to patients who have suffered various neurological injuries of the central nervous system. Stroke ranks as the third leading killer in the United States. People of all ages and backgrounds can have a stroke. At REHAB, we have a large stroke program. We have noticed an increase in young strokes, people between the ages of 45 and 65. For industrialized countries, the mean age of stroke is 75 years, with 20 percent of strokes younger than 65. In recent years, we have seen an increase of about 33 percent of our inpatient stroke population between the ages of 45 and 65. This is a tragedy, for many of them face a lifelong prospect of disability, reduced income levels and challenges at home.
What causes the strokes in the younger population?
This increase has been attributed to methamphetamine use and poor medical compliance for hypertensive (high blood pressure) prescriptions. Methamphetamine use has multiple medical complications: rapid heart rate, irregular heartbeat, increased blood pressure and irreversible, stroke-producing damage to small blood vessels in the brain. Compliance with blood pressure medications is problematic because the medications may be costly or patients don’t experience negative warning symptoms.
|
The good news is that young strokes more commonly have “modifiable” risk factors/ lifestyle choices: tobacco, alcohol and drug use, high cholesterol, obesity and high blood pressure versus “non-modifiable” risk factors - family genetic history and ethnicity. Overall, young stroke patients demonstrate better neurological and functional recovery.
What is the recovery process for young stroke victims?
This population has special problems. Imagine a person about 50 years old. Typically they are married, have children in school, are working and have significant financial obligations. Once that person is “disabled,” even temporarily, their world starts to collapse. Family roles, relationships and responsibilities shift, financial demands loom, and questions regarding their ability to return to competitive employment persist. Stroke-related functional problems include not only physical limitations but also cognitive deficits and emotional changes.
A recent study clarified that age, education, occupation, degree of disability, ethnicity and brain lesion location all influenced outcome.
In the past we depended upon a state agency, the Division of Vocational Rehabilitation, for vocational retraining. But with a cutback of federal/state funds, that avenue has been significantly curtailed. So it has been very difficult for young stroke survivors to really get back on their feet and resume independent control of their lives.
There are several peer support stroke groups for older folks that provide ongoing stroke education and a social support network. Most older stroke patients are retired, have spouses they have lived with for 30 to 40 years, and independent adult children. Life moves at a slower and more predictable pace for them.
However, the younger patients post-stroke have unique psychosocial and supportive needs. The cost to society of stroke in young persons exceeds that of stroke in older persons due to lost productivity and more psychosocial complications. Young strokes benefit from a more aggressive treatment menu of coping skills and problem-solving training, substance abuse and marital/family counseling, and a community commitment of support. Young strokes need to be connected with support organizations and those who share similar experiences.
Is there a range in the effects of stroke?
In a neurological hospital, no two patients are exactly alike. The variables include location of injury or where the stroke occurred in the brain, the size of the injury, whether is was a block (ischemic) or bleed (hemorrhagic), and premorbid health diagnoses such as diabetes or hypertension.
What happens in the body physically when a stroke occurs?
A stroke, or “brain attack,” occurs when blood circulation to the brain fails. Brain cells die from decreased blood flow and the resulting lack of oxygen. There are two broad categories of stroke: those caused by a blockage of blood flow and those caused by bleeding.
How long does it take to recuperate?
Stroke and central nervous system injuries are slow healers. The first benchmark of recovery is approximately six months. It is a dynamic process. Sometimes it seems as if functional recovery plateaus and patients fear that they are not going to get better. It is an internal healing process, unlike a skin wound or a broken bone that you can see.
We used to believe that once brain damage occurred, that was the end of it. But with new diagnostic technology (CT, PET and MRI scans), we now know that dendrites may continue to sprout around the area of injury or that other parts of the brain may assume responsibility for certain functions of the damaged brain, especially in younger people.
Initially, stroke patients are treated in acute-care hospitals. When they are medically stable and ready for rehabilitation, they transfer to an acute rehab facility.
A standard length of stay for a stroke patient at Rehab Hospital of the Pacific is from 10 to 14 days. We work on functional goals such as walking, eating, dressing and toileting.
Typically, our goal is to discharge the patient to home/family/community. Then, outpatient therapies continue the work for four to six weeks.
Eventually, the patient is assigned a home exercise program and encouraged to maintain a daily regimen that includes managing your diet, exercising, medication management, stress management and a healthy, balanced lifestyle.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):