Planning A Healthy Pregnancy
Interviewed by Rasa Fournier
Wednesday - January 11, 2012
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

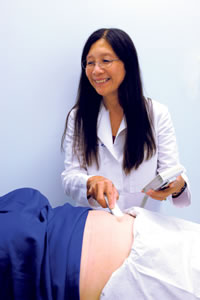
Dr. Mabel Wong
General physician in obstetrics and gynecology at Kaiser Permanente Hawaii
Where did you receive your schooling and training?
I attended the University of California-Davis and did my medical doctorate program at the University of California-San Francisco. I completed my residency training in obstetrics and gynecology at Kaiser San Francisco and joined Kaiser Hawaii in 1994.
How many women do you care for each year during their pregnancy?
For my clinic practice, I care for approximately 100 women per year for their routine prenatal care. I also oversee the care for another 1,000 women per year at Kaiser Permanente’s Moanalua Medical Center for delivery or pregnancy issues.
Is there any special preparation women need when thinking about getting pregnant?
Planning a pregnancy allows women to get preconception care. During a preconception visit we have the opportunity to review a patient’s medical, surgical and social history, family history for both herself and her partner, medications she might be on, and to make sure she is up to date with immunizations. The goal is to have her be as healthy as possible before conception.
Planning for pregnancy also gives women with medical conditions, like diabetes or hypertension, an opportunity to get these concerns under control. If she is on medications or supplements, we can advise changes of medication from those that might be harmful to a fetus to those that are safe in pregnancy.
Family history also helps to identify if there are any underlying genetic risks to the fetus, and also possible underlying maternal medical risks that a patient may not be aware of. Getting rubella (German measles) or varicella (chicken pox) during pregnancy can be harmful to the fetus, so checking to be sure she has immunity to these diseases is important. These vaccinations need to be done before pregnancy. Many women also need an updated vaccination for tetanus, diphtheria and pertussis, which can also be given at a preconception visit.
|
Fetal development starts between three and 10 weeks of gestation, which means that medical problems, medications or behaviors like drinking alcohol or other substance abuse can affect the fetus during this important time of development, before a patient is aware that she’s pregnant. Planning also allows women to be on folic acid supplements to reduce the risk of neural tube defects.
What do you check for during prenatal care?
Our hope is to help pregnant women move through their pregnancies healthy, involved and educated so that they can deliver healthy infants and continue to be healthy themselves. At Kaiser Permanente, our collaborative team of physicians and certified nurse midwives, along with our nurse practitioners, see prenatal care as the way to reach that goal.
Early prenatal care (care in the first trimester) is important to allow us to accurately calculate the gestational age and due date. We also review any risk factors a patient may have, medical or social, which could lead to maternal medical or pregnancy complications so that we can help manage or intervene to reduce these risks.
For example, we order laboratory studies that tell us if she has certain infections, anemia, or is vulnerable to other risks. Additional lab studies may be done depending on her pregnancy history, medical history and general health. During this time we also review healthy diet and weight gain, and generally provide education on the course of pregnancy, danger signs, labor and delivery. Depending on your provider, you may be offered a number of tests throughout your pregnancy that screen for risk of developmental conditions such as Down syndrome, as well as lab studies to evaluate for gestational diabetes (diabetes in pregnancy) and anemia.
During prenatal visits we also listen to fetal heart tones, assess fetal movement, measure blood pressure and weight, screen urine for protein and glucose, and assess fetal growth.
Toward the end of pregnancy it is important to ensure that the baby is in the right position for vaginal delivery. Group B strep is a bacteria that about 30 percent of women are colonized with in the vagina. This is harmless to the mother but can be harmful to the baby, who is exposed to this during birth. So a culture is taken at 35 weeks of pregnancy to determine if mom is a carrier and, if so, she gets antibiotics during labor to protect the baby from infection.
What should a woman do to prepare for delivery?
Being in good physical health is a plus. For new moms, taking a childbirth education course is a good way to prepare for delivery. Identifying your support person for labor your partner, friend or family member and having this person be your coach and advocate is also good planning. Women can also think about whether they want a medicated or non-medicated birth and create their own “wish list” of how they hope their delivery will go.
When might a woman need a Cesarean section?
Cesarean sections are done for a number of reasons. They may be planned for complications of pregnancy like breech presentations, when a baby is poised to come out buttocksor feet-first; placenta previa, which can cause severe bleeding before or during delivery, or other medical conditions in mom or baby for which vaginal delivery would be unsafe. Cesarean sections also are performed during labor if the fetus is showing signs of distress or if the labor is not progressing normally.
Anything else you’d like to mention?
Key messages for women when planning a pregnancy: Maintain a healthy lifestyle with good nutrition. Before conception, stop substances like alcohol or smoking that may harm the fetus or pregnancy, and get preconception guidance from your Ob-Gyn. Once pregnant, get early prenatal care so that your doctor can help educate, support and medically manage your care to ensure a healthy, successful labor and delivery.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):