Quick Calls For Trauma Team
Interviewed by Melissa Moniz
Wednesday - December 26, 2007
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share
|
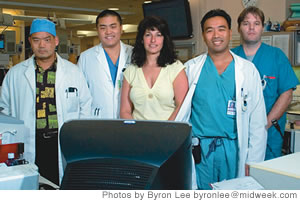
Dr. Hao Chih Ho
Medical Director for Trauma Services at The Queen’s Medical Center
Interviewed by Melissa Moniz
What qualifies a patient as a trauma victim?
Essentially anyone who is physically injured is considered a trauma victim, so it could be injuries from a car crash, a fall, assault, stabbing or gunshot. The Queen’s Medical Center is the only trauma center in Hawaii, so we take care of most of the serious injuries. The ambulance crew will evaluate the patients and bring them here to the trauma center if they have potentially serious injuries. They will communicate with Queen’s Emergency Room, and if the mechanism of injury and condition of the patient satisfies the trauma activation criteria, the trauma team will be paged and we will assemble in the emergency room prior to the patient arriving.
How many people are on the trauma team?
There are 12 people on the trauma team. The trauma team members are all in the hospital 24 hours a day, seven days a week. The team includes: the emergency room physician, the trauma physician (like myself), a surgical resident, the nurses from the emergency room, the emergency room technician, the I.V. team, the radiology technician, the respiratory therapist who manages the ventilator, and the crisis nurse, who documents the vital signs and what kinds of interventions we perform.
What’s an average workday like for you?
When I’m trauma on call, I will start at 7 in the morning and finish at 7 the next morning. We get about 1,700 trauma admissions every year, but the number of patients I see when I am on call is variable. I have had days when I only see one patient, and I’ve had days where I’ve had 16 admissions in one 24-hour shift. When I’m not in the emergency room, I have meetings, paperwork to do and patients who have already been admitted to be taken care of in the hospital.
What are the most stressful situations you are faced with?
When the patients first arrive they can be really badly injured and in shock. Those are the cases in which we have to make quick decisions based on limited information in order to save the patient’s life. You have to be calm in order to do all the things necessary to help the patient, but when the patient is not doing well it’s never easy. Some people are able to handle it better than others, but many people don’t like to be on trauma call because of the uncertainty and the need to make quick decisions under pressure.
Among the trauma team, who makes the call as far as quick decisions?
It would usually be the trauma surgeon who is on call at the time.
What are the most common injuries you see?
Well, we see a lot of fractures, mostly from car crashes. Fractures like broken arms, broken legs and broken pelvises are common. Also common are head injuries mainly from car crashes, but we’re seeing many more head injuries from falls among the elderly. We admitted about 500 patients due to car crashes last year, and about 400 from falls. The car crashes have actually been going down gradually over the last five years, but the falls have been going up.
From the accidents and cases you see, what do you think can be done to prevent some of these injuries?
The common denominator we see is alcohol and drug use. More than half of our patients who come in here test positive for alcohol and/or some other drug. So that is the one thing which, if we could decrease, would really make a big difference in decreasing the number of car crashes and other injuries. Hawaii is, unfortunately, No. 1 in the whole country in terms of alcohol-related traffic fatality rates. We also see quite a few patients who are injured while riding in the back of pickup trucks. They usually get ejected when the truck crashes because they are not restrained. So they are basically flying out and landing on a hard road, causing severe injuries. Also, many of our patients in moped and motorcycle crashes have no helmet on, and so they tend to have a lot of head injuries in addition to the other bodily injuries. Increased helmet use would decrease the number of these devastating head injuries.
Do you see a lot of cases where children and infants are in neither a booster seat nor car seat, or not properly strapped in?
We do see quite a few of those. We (The Queen’s Medical Center) have a keiki car seat fitting station. So we try to educate the public on how to properly secure the car seat in the car, and how to properly secure the child in the car seat. We’ve had car crashes where the infant in the car crash is ejected with the seat. And that’s because it wasn’t fastened properly. We also see a lot of children who are run over by a car backing up. Those are some of the most tragic situations that we encounter.
Is there an increase in the number of patients you see during the holiday season?
Yes. We do see an increase near the holiday season because people tend to indulge a little bit more and make poor decisions.
Have you seen any miracles happen before you eyes in the E.R. or operating room?
We don’t really see any miraculous recoveries. There are patients with injuries that may not be as bad as we initially think and then end up doing well. There are patients who appear initially to have really bad head injuries but it turns out they’re just intoxicated. So those are not really miracles.
What do you like most about what you do?
I like to be able to make a difference and help some of these patients who are injured - to help them get back to the life they had before the injuries.
What advice do you have for someone who is looking into becoming a trauma physician?
You need to be able to work not-so-regular hours. You never know when an accident is going to happen, and most of them do come in the middle of the night. You have to be able to accept that when the patient first comes in you need to make very rapid decisions on very limited information, so you have to be able to deal with that uncertainty and stress. Patients can be very badly injured, and you have to be able to deal with the fact that you will not be able to save some of them.
How do you work with the families in situations where they want to see their loved one who has been admitted into the E.R. and/or wants questions answered, etc.?
Usually we would allow the family or at least one or two members to come and see the patient if the patient is relatively stable. If the patient is really unstable, and we’re doing a lot of different things, then usually we will not have the family go in because they might get in the way during some of the procedures we are performing.
What percentage of the trauma center patients are Neighbor Island and how many are Oahu?
Last year we admitted a total of 1,668 patients, with 245 of them from the Neighbor Islands. Most of them came from the Big Island (169). The Big Island has been sending us an increasing number of patients every year. It’s probably because the population is growing fastest there, and there is a shortage of specialists, especially orthopedic surgeons and neurosurgeons. Right now we have two air ambulance services that fly Neighbor Island patients to Queen’s.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):