The Dangers Of Sleep Disorders
Interviewed by Melissa Moniz
Wednesday - December 16, 2009
E-mail this story | Print this page | Comments (0) | Archive
 Del.icio.us Share
Del.icio.us Share

Dr. James Kohan
Medical director of Pacific Sleep Tech
Where did you receive your schooling and training?
I went to University of Virginia for undergraduate and medical school. I did my medical residency in Brooklyn, N.Y., and I did my fellowship in pulmonary medicine in Rochester, N.Y. When I was there, they were just starting a sleep lab, and at the time there were only five sleep labs in the country (there are now 5,000 in the United States) and that’s the fellowship that I chose to do. That’s how I got into sleep. Since then, the contribution of sleep disorders in both health and disease became very well-recognized and accepted. Initially we were monitoring people’s breathing when they sleep because it’s been known for about 40 years that when people with lung disease sleep, that was the worst time for their blood oxygen levels. What’s happened is that the disease called sleep apnea became the driving force behind sleep medicine. When we talk about sleep apnea, it’s a risk factor for heart disease and stroke. So if you have sleep apnea and you don’t treat it, then you have a four times greater risk of having a heart attack. The problem with sleep apnea is because you’re sleeping you don’t know it’s occurring, so the people who have it are the last to know.
How long have you been practicing?
I’ve been in medicine for 25 years and have been in Hawaii for the past six years.
Can you talk about the services offered at Pacific Sleep Tech?
We evaluate basically two types of problems: people who are too tired and people who have insomnia or trouble sleeping. We also see patients who do bizarre things when they sleep like sleep walk, and people who have sleep-wake problems like swing-shift workers and jet-lag sufferers.
We pride ourselves in having state-of-the-art equipment and four-star accommodations. A lot of sleep labs have very small rooms and beds, and patient comfort is compromised. Here you can relax and pretty much have as good a sleep as you would have at home, or even better. Our staff is experienced and well-trained, and their professionalism helps put people at ease, and that’s the important thing for a successful sleep study.
|
For the problems that you mentioned, are there treatments for each?
The good thing about sleep medicine is that you can help people. So almost everything that you find wrong you can do something about it. With insomnia, it’s not always just sleeping pills because usually that’s a short-term fix. So we work to correct behaviors and improve what we call sleep hygiene. For people who are too tired, we can almost always help them, including with sleep apnea and snoring.
Can you explain what sleep apnea is?
When we sleep the brain goes through a series of sleep stages: two stages of light sleep, one of deep sleep and then dream or REM (rapid eye movement) sleep. Deep sleep is the best sleep for resting/renewing the body, and REM is the most important for regenerating brain function, such as thinking, concentration, memory and mood. In deep sleep the muscles all relax, and in REM the muscles are paralyzed (so we don’t act out our dreams). The back of the throat down to the level of the voice box is a muscular channel, and like the rest of the body, these muscles relax during deep sleep and are paralyzed during REM.
Snoring is the sound of the relaxing throat muscles vibrating and touching each other: The louder the snore, the smaller the opening. Apnea is when the throat size narrows by 50 percent or more for at least 10 seconds, because when that occurs, the lungs run out of air. This causes the blood oxygen level to fall and the blood pressure to rise. When this happens, the brain notices and bumps itself back into light sleep, which awakens the throat, but not the sleeper. So with sleep apnea, the interrupted deep sleep and REM cause daytime fatigue (with resultant tendency to make mental and physical mistakes), and the frequent bouts of low oxygen and high blood pressure promote heart attacks and strokes.
The good news is that when we do a sleep study in the lab, we are able to accurately measure sleep stages, breathing patterns and oxygen levels, cardiac monitoring and muscle activity in order to make a diagnosis of sleep apnea and initiate treatment, which is then prescribed for home.
Is sleep apnea associated with obesity?
Being overweight does make you more prone to sleep apnea. Most people with sleep apnea are over-weight, but not always, because it has to do with the anatomy of the throat. The reason why weight is important is because when we go into deep sleep and dream sleep, our chest and belly muscles are relaxed/paralyzed, and this squashes the lungs, resulting in a faster lost of air reserve.
So gaining weight makes it worse, and it’s known that if someone with sleep apnea loses weight then it gets better. However, when they have sleep apnea, it’s hard for them to lose weight because they are too tired to exercise and tend to sit around more. There’s also a chemical that your brain squirts out that stops you from eating, but when you have sleep apnea the brain doesn’t secrete that chemical. The other thing that adds to the eating is that when you’re very tired you have a tendency to eat snacks and sugary foods to give you a boost. So they tend to get all these extra calories.
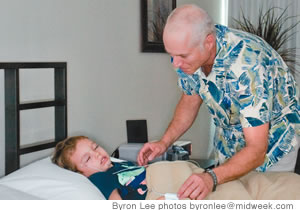
Do these types of sleep disorders affect children?
With children, there’s an emerging trend in sleep apnea. Children who had sleep apnea used to be less than 5 years old and it was related to big tonsils. And it was ages under 5, because after age 5 usually your tonsils start to shrink. Now studies show that there’s a second group of children who are showing sleep apnea, and that’s the early teenagers (ages 12-15), and it’s related to kids being overweight. It’s the same thing where the belly squashes the lungs and the breathing muscle has to overwork to push that belly off the lungs, and that causes the throat to collapse.
Are disorders diagnosed within one session?
Sometimes, besides a consultation, it’s just one night in the lab. But, in general, it’s one night to make a diagnosis and then a second night to start the treatment and adjust it to see if it corrects the problem. But if they come in and the sleep apnea is severe, occurring even in light sleep, then we’ll go in and treat them right away and will do two nights in one.
What do you see as the future of sleep disorder testing and treatment?
One thing is that people with sleep apnea, probably about 70 percent of them, still don’t know it. So there are a lot of undiagnosed patients, especially here in Hawaii. I think it’s important to identify people who have this problem, and I think once that’s done the trend is going to be to get the sleep lab into the home. Soon the technology will be good enough to allow valid studies at home.
The other thing I think will happen is that sleep will become a bigger part of basic health education. So people will be more aware and hopefully give more attention to their sleep. The problem is that as societies become more civilized people sleep less and widespread sleep deprivation occurs. We can’t keep doing that because it’s bad for our health.
E-mail this story | Print this page | Comments (0) | Archive
Most Recent Comment(s):